Cardiometabolic disease costs the US healthcare system 45B dollars every year.
Our health system has traditionally approached cardiometabolic disease (heart disease, diabetes, stroke, high blood pressure) via pharmaceutical treatment and surgery. While these treatments continue to advance, the treatment options are becoming less efficient at lowering death rates. Why?
The decline of treatment efficiency could be due to the fact that pharmaceutical and surgical approaches fail to address the root cause of poor cardiometabolic health: proper diet. Alternative approaches that use dietary modification to correct poor diet are necessary to reduce the cost, frequency and growing impact of cardiometabolic diseases.
Food As Medicine (FAM) is a type of dietary modification that prevents and treats cardiometabolic disease by removing the barriers to a healthy, well balanced diet. The FAM approach allows for dietary modification by addressing the following challenges that make consumption of a proper diet difficult: Food Insecurity, Insufficient Access to Nutrition Education and Consistent Behavior Change.
Download The Complete Whitepaper: Opportunities in Food as Medicine
Challenge 1: Food Insecurity
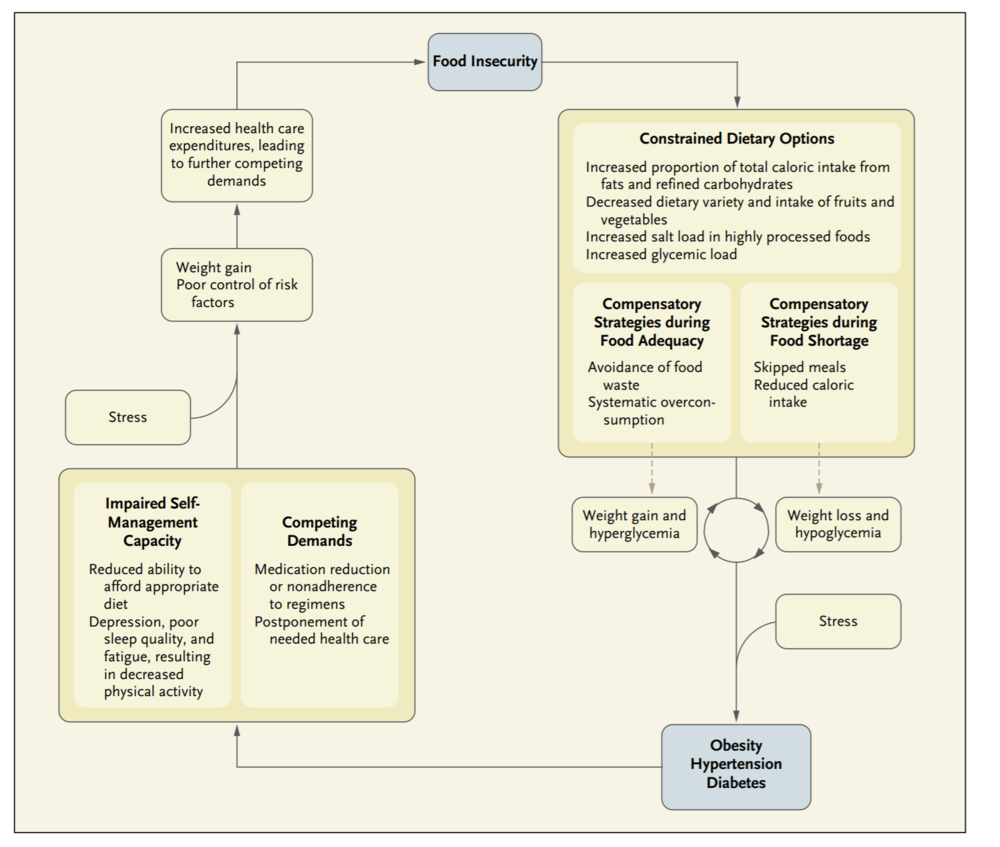
Food insecurity is a social/economic condition where access to nutritious food is limited or uncertain. In the United States, 40M people are food-insecure. Those who are food insecure are stuck in a cycle of increased rates of cardiometabolic disease and higher healthcare costs due to lack of access to healthy foods. Breaking the cycle of food insecurity would yield lower rates of cardiometabolic disease and reduce healthcare costs across the board.
Food insecurity leads to increased rates of cardiometabolic disease and higher healthcare costs.
Challenge 2: Insufficient Access to Nutrition Education
A recent Food Information Council Report indicates that 80 percent of consumers find conflicting information about food and nutrition, while 59 percent say the massive amounts of data about food makes them doubt their nutritional decisions.
Consumers need a trustworthy resource (such as a care provider) to cut through the conflicting information and provide clear dietary instructions. Unfortunately, proper dietary information is tough to sift through for a few reasons:
- Many doctors are not properly educated to teach patients about proper diet. On average, <20 hours of medical school is spent teaching future physicians about nutrition. Additionally, only 14 percent of residents report feeling adequately trained to offer solid nutritional guidance to their patients.
- Doctors are not incentivized to teach patients about proper diet. In today’s current healthcare reimbursement system dominated by fee-for-service, physicians aren’t rewarded for the time spent with patients to offer nutritional guidance—with their perpetually busy schedules, doctors aren’t inclined to spend their time offering “free” information.
- Other care providers such as Registered Dietitians (RDs), who are trained to formulate dietary plans for consumers, are difficult to access. Access to RDs is difficult for two reasons:
- In order for consultations with RDs to be reimbursed, many consumers (such as those on Medicare) require a physician referral. This means patients need doctors to be aware of/understand the need for a referral. It takes time to schedule an appointment and explain their situation to a physician.
- If the patient is able to obtain a physician referral, a care-coordination obstacle usually occurs as the patient must then schedule and attend a separate consultation because most RDs are not located in primary care offices.
The care-coordination gaps present a large problem, exemplified by the fact that of the 15M Medicare members who could have benefited from consultations with an RD, only 100K took advantage in 2017.
Challenge 3: Consistent Behavior Change is Difficult
Many individuals struggle with consuming a proper diet despite overcoming the challenges of food insecurity and insufficient nutrition education. Even when consumers intend to eat better, they often fail to change their dietary behavior because of psychological and environmental barriers.
- Consumers fail to make consistent dietary changes because they eat mindlessly and consume out of habit. In a study by Gardner et al., (2011), it was found that roughly 20 percent of variation in nutrition-related behavior is due to a person’s habits.
- People feel they lack the self-efficacy to make appropriate dietary changes, i.e.: they feel they do not have the cooking skills or the time to cook, and therefore feel less empowered to change their diet.
Other barriers to consistent dietary change include a person’s social and physical environment. People are more likely to continue eating poorly if they do not have support from their social group. Similarly, it’s hard to make a change if the physical environment is composed of poor nutritional options.
Solutions to Dietary Modification
Interested in learning more about how to combat the challenges of dietary modification? JSF’s whitepaper “Opportunities in Food as Medicine” takes a deep dive into the challenges and solutions of dietary modification, the maturity of the market for Food as Medicine and outlines JSF’s predictions for market developments and recommendations of FAM opportunities.
While pharmaceutical and surgical treatments continue to advance, these treatment options are becoming more expensive and less efficient at lowering death rates. Is this occurring because pharmaceutical and surgical approaches fail to address a root-cause?
Download the Food as Medicine whitepaper to learn about:
- The challenges our health system is currently facing when it comes to cardiometabolic disease
- How using food as medicine can drive dietary modification to reduce cardiometabolic disease
- Jumpstart’s take on where we think this industry is headed